Ocular Scanning in ICH
CASE
A 20-year-old female presents to the emergency department (ED) with a chief complaint of a headache. Her headache started 8 days ago and is described as bifrontal. It is positional and gets worse when she bends forward but improves when she is sitting or standing. She had presented to 3 other EDs prior to this visit for her symptoms, and each time she was discharged with an intractable headache after receiving a migraine cocktail to no effect. Associated symptoms included blurry vision with floaters, decreased appetite, and neck stiffness. On physical exam she was afebrile with hypertension to 150/99, difficulty tracking on visual field testing, and 4/5 strength in her upper extremities bilaterally. The rest of her neurological exam was unremarkable. The differential included idiopathic intracranial hypertension, and meningitis so an LP was performed which showed an opening pressure of 50 cmH20 with clear fluid. The patient reported symptomatic relief following the removal of 20cc of CSF and she was admitted to neurology. Given her complaint of vision changes an ocular ultrasound was performed to assess the optic nerve.
DIAGNOSIS
Idiopathic Intracranial Hypertension
DISCUSSION
Methodology
The ocular ultrasound examination procedure consisted of placing a non-adhesive sterile dressing over the closed eye and placing ultrasound gel over the dressing. Cold gel is preferred if available as it holds form over the eye, rather than dripping down the patient’s face. Patient should be in the semi-recumbent position. Place the high frequency linear probe over the eye and scan through the entire globe in two planes (sagittal with the probe marker to the patient’s head and transverse with the probe marker to the patients right). Consider bracing your hand on the bridge of the nose to avoid any excess pressure on the eye, as this could cause a vasovagal response.
Figure 1. Sonographic eye anatomy. Courtesy of ACEP Sonoguide [1]
Normal Eye Ultrasound Anatomy
In a normal eye the vitreous humor will appear anechoic, or black. The cornea, iris, and lens contour will appear as hyperechoic, or white, structures. Just deep to the eyelid is the cornea and the anterior chamber. Instructing the patient to move their eye can improve visualization of certain structures. A pupillary light reflex can be assessed by shining a light in the exposed eye and watching for ciliary muscle contraction in the contralateral eye. The far field concave face of the globe should be smooth and uninterrupted. Deep to the globe lies the optic nerve, which normally presents as a hypoechoic vertical streak. The optic nerve sheath may be visualized as parallel hyperechoic streaks lateral to the nerve.
Measurement of the Optic Nerve Sheath Diameter (ONSD)
The ONSD can be measured 3 mm back from the rim of the globe and should measure approximately 5 mm or less in healthy adults. ONSD is commonly underestimated when the operator measures the width of only the hypoechoic area. The borders of the optic sheath appear as thin hyperechoic parallel lines and accurate measurement should span the entire space between those lines–from one hyperechoic structure to the other. However, because the sheath is so thin it is often difficult to visualize clearly on ultrasound. This underscores the notion that the specificity of the study improves with larger ONSD values, as an ONSD of 9mm is likely abnormal even if undermeasured. Remember that the ultrasound probe beam should not be at an angle to the optic nerve but should be aimed directly at the nerve. An accurate measurement is possible but takes some attention to detail.
Case Resolution
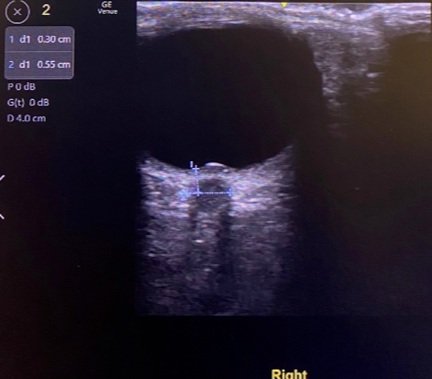
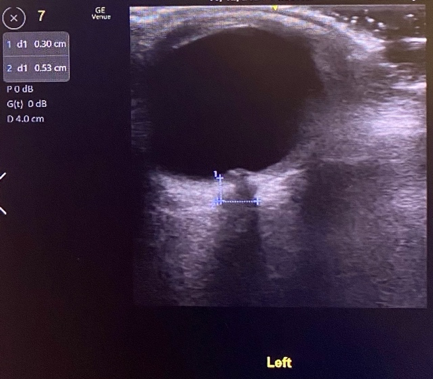
Our patient’s ocular ultrasound, Figures 2-3, reveals an intact globe, without evidence of retinal detachment or lens dislocation. However, ONSD measurement showed enlargement to 5.5mm in the right eye and 5.3mm in the left eye. Enlargement of the optic nerve sheath may be indicative of increased intracranial pressure, which was confirmed on lumbar puncture in this patient. This patient’s ocular scan also showed a hyperechoic structure that disrupted the inner contour of the globe in the far field, referred to as “nippling” of the optic nerve. Nippling of the optic nerve is frequently indicative of papilledema but can often be confused with optic nerve head drusen, which are hyperechoic hyaline bodies that form due to calcification of optic nerve axons. Optic nerve head drusen is distinguished from papilledema on ultrasound by a normal ONSD (<5mm). Additionally, patients with optic nerve head drusen are usually clinically asymptomatic whereas papilledema usually presents with visual changes, as seen in this patient. Ultrasound videos of papilledema and optic nerve head drusen are provided below for comparison.
RELEVANT VIDEOS
1. Optic nerve nippling on ultrasound in our patient with intracranial hypertension:
https://youtube.com/shorts/ahz9dMElv3k?feature=share
2. Asymptomatic Optic Nerve Head Drusen:
KEY TAKE-AWAYS
· Ultrasound is an effective, non-invasive tool for assessing the structures of the eye in ophthalmologic emergencies such as retinal detachment, eye trauma, or vision changes.
· Ultrasound measurement of the ONSD should be 5mm or less when measured 3mm back from the globe in a healthy adult
· Papilledema can be visualized as outpouching of the optic nerve into the vitreous humor, termed nippling.
· Opening pressure measurement on lumbar puncture is still the primary method of definitively diagnosing elevated intracranial pressure, but bedside ultrasound is an effective, non-invasive tool to access for ocular signs of elevated intracranial pressure.
AUTHOR: Danielle Charles-Chauvet, MS4
FACULTY REVIEWER: Kristin Dwyer, MD
REFERENCES
1. American College of Emergency Physicians. (2020, August 18). Ocular emergencies. Sonoguide | Advanced Sonography: Ocular Emergencies. Retrieved October 17, 2021, from https://www.acep.org/sonoguide/advanced/ocular-emergencies/.
2. 5 Minute Sono·February 14, 2020·1 min read. (2020, February 19). Optic nerve sheath diameter. Core Ultrasound. Retrieved October 17, 2021, from https://www.coreultrasound.com/onsd/.